Lassa fever is a dangerous virus spread by rats that attacks the body’s blood vessels and often causes uncontrolled bleeding from the nose, mouth, or eyes. It quietly spreads to hundreds of thousands of people in West Africa every year, but most people around the world don’t know much about it. While most infections go unnoticed, several infected persons end up with organ failure, deafness, or death, especially in places where health care is weakest.
As of early 2026, Nigeria is managing an ongoing Lassa fever outbreak, with 51 deaths recorded in the first six weeks of 2026. With a majority of cases concentrated in Ondo, Bauchi, and Edo states, Lassa fever presents a high case fatality rate of 18.4%. It primarily affects young adults aged 21-30, with most transmission occurring during the dry season.
What Lassa Fever Is and Where It Strikes
Lassa fever is caused by Lassa virus, an arenavirus carried mainly by the multimammate rat Mastomys natalensis, which commonly lives in and around houses in West Africa. An estimated 200,000–500,000 infections and up to 10,000 deaths occur annually, with Nigeria, Sierra Leone, Liberia, and Guinea bearing the greatest burden.
In the past, infections were exclusive to rural areas, but in recent times, it has become pronounced in suburban regions due to environmental changes and larger rodents’ habitats.
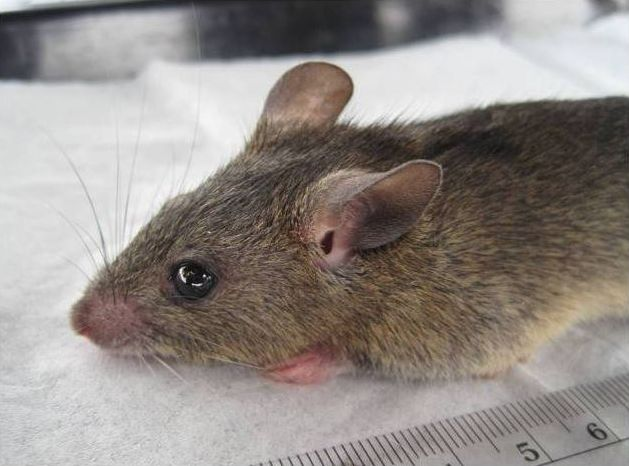
Picture: The Natal multimammate rat (Source: Wikipedia)
How It Spreads and Whom It Hurts Most
Primary infection occurs when food, water, or household surfaces are contaminated with urine or feces from infected rodents. Humans can also get infected when they handle, hunt, or eat these infected rodents. Secondary human‑to‑human spread happens through contact with blood and body fluids, especially in hospitals lacking proper protective equipment.
Around 80% of infections are asymptomatic or mild; the remaining 20% can progress to severe multi‑organ disease with bleeding, shock, kidney injury, and brain involvement. Hospital case‑fatality can reach 15–30%, and pooled estimates for severe hospitalized cases are about 19–34%. Pregnant women, especially in late pregnancy, and their newborns face the highest risk of death. Up to a third of survivors develop some degree of permanent deafness, with major social and economic consequences.
Diagnosis, Treatment, and Prevention
Early signs of the disease include fever, weakness, headache, sore throat, and sometimes coughing or abdominal pain. Since these signs resemble those of malaria, typhoid, and other fevers, Lassa fever is usually not diagnosed early. To confirm the presence of this disease in a patient, special investigations such as RT-PCR and ELISA must be carried out.
For this purpose, the antiviral drug ribavirin is effective if taken early in the course of severe disease. However, effective healthcare is not always available, especially at the right time. Unfortunately, no vaccine is currently available for this disease. However, several vaccine candidates, such as rVSV, DNA vaccine, and measles virus vectors, have shown promise in animal studies as well as early human trials.
However, for effective control of this disease, a combination of interventions is needed. These include improving living conditions, such as housing and food storage to keep rodents away, effective infection control practices in clinics, effective health education campaigns tailored for the community, as well as surveillance and quick diagnostic services.
Social Impact and the “Silent” Nature of the Scourge
Aside from the health impact of Lassa fever, it also brings fear and poverty. In some cases, Lassa fever causes miscarriages and deafness, which may result in divorce and poverty. In addition, because of the expenses of Lassa fever treatment, some families may have to choose between food and medicine.
Because most cases of Lassa fever are mild and surveillance systems are inadequate, it makes it difficult to know the actual burden of Lassa fever in Africa and other endemic areas. In fact, according to meta-analyses, there are significant gaps in basic parameters such as infection rates, transmission dynamics, and geography of Lassa fever infection, indicating how little attention Lassa fever receives despite its impact.
Conclusion
Lassa fever is a rodent-borne viral hemorrhagic fever that quietly infects hundreds of thousands of people in West Africa. The effects range from various disabilities to fatal cases.
It thrives in poor areas, especially due to bad housing conditions and inadequate health infrastructure. In its early stages of infection, it presents itself as a common tropical fever. It has no vaccine and no cure, and its most potent weapon against it is early diagnosis and robust infection control practices in hospitals. In addition, rodent-proof food storage practices such as food storage in airtight plastic containers and effective sensitization of communities are crucial in controlling Lassa fever at homefront levels. Until all these measures are put in place, Lassa fever will continue to quietly plague some of the world’s most vulnerable populations.
Sources
Nigeria Centre for Disease Control and Prevention. (2025, December). Lassa fever situation report, epi week 51: 15th-21st December 2025. https://ncdc.gov.ng/themes/common/files/sitreps/070ffa8b118e6170bb61854b22b06cb.pdf
Asogun, D., Günther, S., Akpede, G., Ihekweazu, C., & Zumla, A. (2019). Lassa Fever: Epidemiology, Clinical Features, Diagnosis, Management, and Prevention. Infectious disease clinics of North America, 33 4, 933-951. https://doi.org/10.1016/j.idc.2019.08.002.
Uppala, P., Karanam, S., Kandra, N., & Edhi, S. (2025). Lassa fever: A comprehensive review of virology, clinical management, and global health implications. World Journal of Virology, 14. https://doi.org/10.5501/wjv.v14.i3.108405.
Efe, U., Edward, E., Chinaza, A., Emmanuella, O., & Chidinma, N. (2024). Lassa Fever: A Mini Review of Clinical Features, Diagnosis, and Treatment. Asian Journal of Research in Infectious Diseases. https://doi.org/10.9734/ajrid/2024/v15i8363.
Asogun, D., Arogundade, B., Unuabonah, F., Olugbenro, O., Asogun, J., Aluede, F., & Ehichioya, D. (2025). A Review of the Epidemiology of Lassa Fever in Nigeria. Microorganisms, 13. https://doi.org/10.3390/microorganisms13061419.
Besson, M., Pépin, M., & Metral, P. (2024). Lassa Fever: Critical Review and Prospects for Control. Tropical Medicine and Infectious Disease, 9. https://doi.org/10.3390/tropicalmed9080178.
Garry, R. (2022). Lassa fever — the road ahead. Nature Reviews. Microbiology, 21, 87 – 96. https://doi.org/10.1038/s41579-022-00789-8.
Pal, M., Areda, N., & Lema, A. (2022). A Comprehensive Review on Lassa Fever in Africa: Epidemiology, Diagnosis, Prevention and Control. International Journal of Healthcare and Medical Sciences. https://doi.org/10.32861/ijhms.83.35.43.
Rauf, S., Ahmed, R., Jamalvi, S., Ali, S., Kumar, N., & Haque, M. (2025). Lassa fever: urgent measures for protection and control in West Africa. International Journal of Surgery: Global Health, 8. https://doi.org/10.1097/gh9.0000000000000528.
Islam, M., Akash, S., & Rahman, M. (2023). Epidemiology, symptoms, transmission, prevention, treatment, and prospects of the Lassa fever outbreak: a potential study. International Journal of Surgery (London, England), 109, 531 – 533. https://doi.org/10.1097/js9.0000000000000013.
Doohan, P., Jorgensen, D., Naidoo, T., McCain, K., Hicks, J., Mccabe, R., Bhatia, S., Charniga, K., Cuomo-Dannenburg, G., Hamlet, A., Nash, R., Nikitin, D., Rawson, T., Sheppard, R., Unwin, H., Van Elsland, S., Cori, A., Morgenstern, C., Imai-Eaton, N., Morris, A., Forna, A., Dighe, A., Vicco, A., Hartner, A., Lambert, B., Daniels, B., Whittaker, C., Santoni, C., Geismar, C., Dee, D., Knock, E., Unwin, E., Thompson, H., Dorigatti, I., Routledge, I., Wardle, J., Skarp, J., Hicks, J., Parchani, K., Fraser, K., Drake, K., Geidelberg, L., Cattarino, L., Kusumgar, M., Kont, M., Baguelin, M., Guzman, P., Liétar, P., Christen, P., Nash, R., Fitzjohn, R., Sheppard, R., Johnson, R., Leuba, S., Ruybal-Pésantez, S., Radhakrishnan, S., Naidoo, T., & Perez, Z. (2024). Lassa fever outbreaks, mathematical models, and disease parameters: a systematic review and meta-analysis. The Lancet. Global health, 12 12, e1962-e1972. https://doi.org/10.1101/2024.03.23.24304596.
Medugu, N., Adegboro, B., Babazhitsu, M., Kadiri, M., & Abanida, E. (2023). A review of the recent advances on Lassa fever with special reference to molecular epidemiology and progress in vaccine development. African Journal of Clinical and Experimental Microbiology. https://doi.org/10.4314/ajcem.v24i2.3.
Okwuraiwe, A., Onyeaghala, C., Ozoude, O., Suleiman, M., Abdu-Aguye, S., Ezekwelu, N., Oyeniyi, T., Jegede, A., Egwudo, A., Okeke, O., Abodunrin, O., Akinsolu, F., & Sobande, O. (2025). Clinical Outcomes of Severe Lassa Fever in West Africa: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health, 22. https://doi.org/10.3390/ijerph22101504.
Akafa, T., John, A., Oladele, G., & Umaru, I. (2025). Persistent Threat of Lassa Fever in Nigeria: Epidemiology, Challenges, and Strategies for Effective Management. African Journal of Medicine, Surgery and Public Health Research. https://doi.org/10.58578/ajmsphr.v2i2.5517.
Wang, Y., Wen, X., Li, D., Fan, S., Zhou, X., Yan, K., Cao, J., Li, J., Wei, R., Liu, H., Wu, W., Zheng, S., Jiang, R., Peng, Y., Feng, Y., Xiang, N., & Zhou, J. (2025). The First Imported Case of Lassa Fever — China, 2024. China CDC Weekly, 7, 400 – 404. https://doi.org/10.46234/ccdcw2025.066.
Grace, J., Egoh, I., & Udensi, N. (2021). Epidemiological trends of Lassa fever in Nigeria from 2015-2021: A review. Therapeutic Advances in Infectious Disease, 8. https://doi.org/10.1177/20499361211058252.
Wolf, T., Ellwanger, R., Goetsch, U., Wetzstein, N., & Gottschalk, R. (2020). Fifty years of Imported Lassa Fever: A Systematic Review of Primary and Secondary cases. Journal of Travel Medicine. https://doi.org/10.1093/jtm/taaa035.
Hartnett, J., Boisen, M., Oottamasathien, D., Jones, A., Millett, M., Nelson, D., Muncy, I., Goba, A., Momoh, M., Fullah, M., Mire, C., Geisbert, J., Geisbert, T., Holton, D., Rouelle, J., Kannadka, C., Reyna, A., Moses, L., Khan, S., Gevao, S., Grant, D., Robinson, J., Happi, C., Pitts, K., Garry, R., & Branco, L. (2015). Current and emerging strategies for the diagnosis, prevention, and treatment of Lassa fever. Future Virology, 10, 559-584. https://doi.org/10.2217/fvl.15.41.
Ogundele, G., Jolayemi, K., & Bello, S. (2025). Lassa fever in West Africa: a systematic review and meta-analysis of attack rates, case fatality rates and risk factors. BMC Public Health, 25. https://doi.org/10.1186/s12889-025-24377-6.

